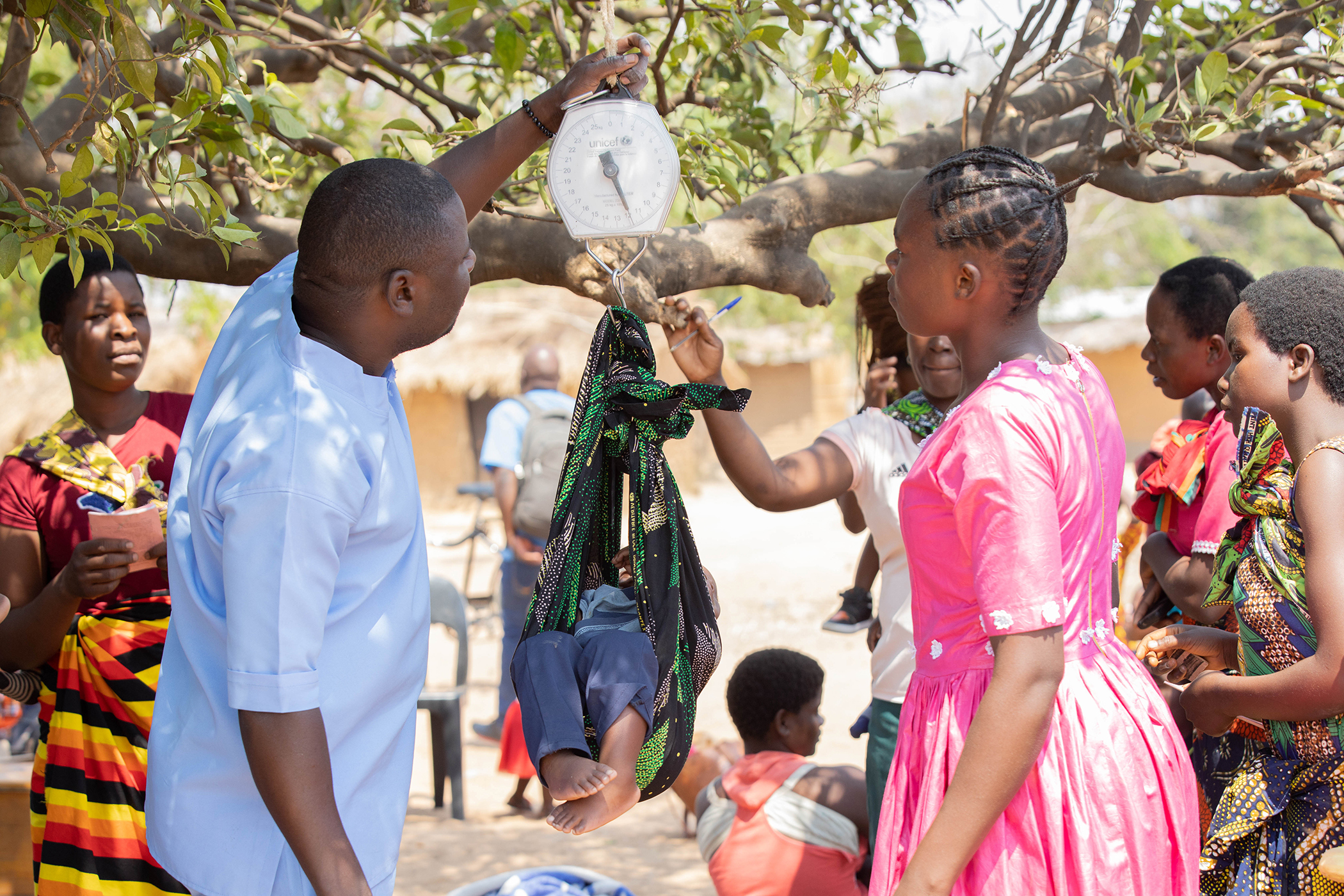Sponsored by Action for Global Health
One year ago, the UK government announced it would reduce its aid commitment from 0.5% to 0.3% of national income.
It was the second major reduction in four years. In 2021, the UK reduced aid from 0.7% to 0.5%.
Taken together, these decisions are set to reshape the UK’s role in advancing health for all — against a backdrop of colliding crises.
The risks are not theoretical.
When UK health funding was reduced in 2021, around 200 health facilities in South Sudan — including major hospitals — lost support. Clinics closed. Health workers went unpaid. Access to care narrowed in a country already facing conflict, displacement and climate shocks.
In fragile settings, funding reductions can mean fewer vaccinations, shortages of essential medicines and increased pressure on maternity wards. In refugee camps in Bangladesh, underfunding has been associated with rising malnutrition and increasing disease risk. In Yemen and Afghanistan, feeding centres and paediatric units have reported operating beyond capacity during peak periods.
Women and girls are often disproportionately affected. Analysis by Save the Children UK suggests that reductions to UK funding for family planning and nutrition could mean tens of millions fewer women and girls receiving support compared with 2019 levels — with implications for maternal health and child survival.
At the same time, global pressures are intensifying. Climate change is contributing to disease outbreaks and extreme weather. Conflict continues to drive displacement and hunger. Amid these compounding crises, the US administration’s dismantling of USAID triggered a wider retreat from global health — undermining hard-won global health cooperation at a critical moment.
Disease outbreaks, antimicrobial resistance and climate-driven health shocks do not respect borders. In a world of shared risk, retreating from collective action undermines preparedness. Protecting access to care everywhere means recognising that solidarity is a responsibility, not a gesture — and that global health cannot be safeguarded in isolation.
Against that backdrop, the move from 0.5% to 0.3% signals that the UK is stepping back at a moment when cooperation and partnership is most needed.
The question is how the UK contributes fairly to the collective effort to protect health for all.
Click here to join our movement for health for all
Here are three practical ways forward.
In Mvolo County, South Sudan, we visited Helen, a former student at Maridi Insititute of Health Sciences, who now heads the labour unit at the local facility. Photograph by Amref Health Africa/Steve Kagia
1. Put people and global solidarity first
Health systems are built by the people who run them — the nurses, midwives, community health workers and local leaders who keep care going every day.
Covid showed what happens when the world is underprepared — and what is possible when countries act together. When investment stalls, progress can unravel fast.
The UK helped build many of the partnerships now at risk, including Gavi, the Vaccine Alliance, which expands access to immunisation, and the Global Fund to Fight Aids, Tuberculosis and Malaria, which supports disease-control programmes worldwide. The UK-founded Fleming Fund, created to tackle the growing threat of antimicrobial resistance, has been closed altogether.
Cutting back again, just as global needs are rising, is not a neutral act. If global solidarity means anything, it must show up in sustained support for care, vaccines and the health workers that communities rely on.
2. Tackle the debt crisis constraining health budgets
Many countries facing severe health challenges spend substantial portions of public revenue on debt repayments. Analysis from Results UK indicates that the 16 countries most affected by food crises spend nearly twice as much servicing external debt as they do on health.
When debt servicing absorbs fiscal space, less funding is available for essential health services, doctor and nurse salaries and essential medicines.
The UK is not only reducing its aid budget, it is also a key actor in the financial institutions that shape global debt rules. Failing to push for fairer restructuring means leaving countries trapped between servicing creditors and funding healthcare. Supporting more flexible debt restructuring and mechanisms such as debt-for-health or climate swaps could help countries redirect resources toward frontline services without increasing unsustainable borrowing.
Community Health Worker Fanizo Simenti (known as Simenti) weighs Stanley as his mother Gribeta Ventula (29) looks on. This is during an outdoor, community health outreach done under a lemon tree in Katenje, Kasungu, Central Malawi. Distances to health centres are often long making access to health services difficult to communities. Photograph by Amref Health Africa/Amaru Photography
3. Put health at the centre of climate action
Climate change is already driving disease outbreaks, heat stress and food insecurity. Yet only a tiny fraction of global climate finance is currently spent on building climate-resilient health systems.
Communities on the front line of climate impacts need health systems that can withstand floods, droughts and rising disease risks. That requires investing in climate-resilient clinics, trained health workers and early warning systems.
The UK has committed billions to climate finance. Making health a core priority within that funding would reflect the simple reality that climate justice and health justice are inseparable. The question is not whether we can afford to act — but whether we choose to.
Top photograph © UNICEF/Ilvy Njiokiktjien