I gave evidence to the Covid inquiry in September 2024. Aside from getting through the pandemic itself, it was one of the hardest things I’ve ever had to do. I cried on the stand; I couldn’t stop myself.
NHS England seconded me as national clinical adviser in emergency preparedness resilience and response in mid-March 2020. I thought the position would last for three or four months. I was still there three years later.
I set up and ran a programme of peer support visits, taking small teams of frontline clinicians into hospital after hospital across the country. We went wherever we were asked to go. We were there to provide support by giving people the chance to share what they were going through, and to have their remarkable achievements – won against terrible odds – affirmed.
At the same time it gave the national strategic team insight that helped them better understand how close these hospitals were to the limits of their capacity.
Baroness Hallett’s report, “The impact of the Covid-19 pandemic on the healthcare systems of the United Kingdom”, released on 19 March, finds that the NHS was in a fragile state even before Covid arrived, neither properly resourced nor staffed to deal with the tidal wave of demand that was to come.
Because of that the NHS was overwhelmed in many places and at many times during the pandemic. That it didn’t collapse entirely is testament to the extraordinary efforts of the NHS teams who delivered the care under extraordinary circumstances. But that came at a price.
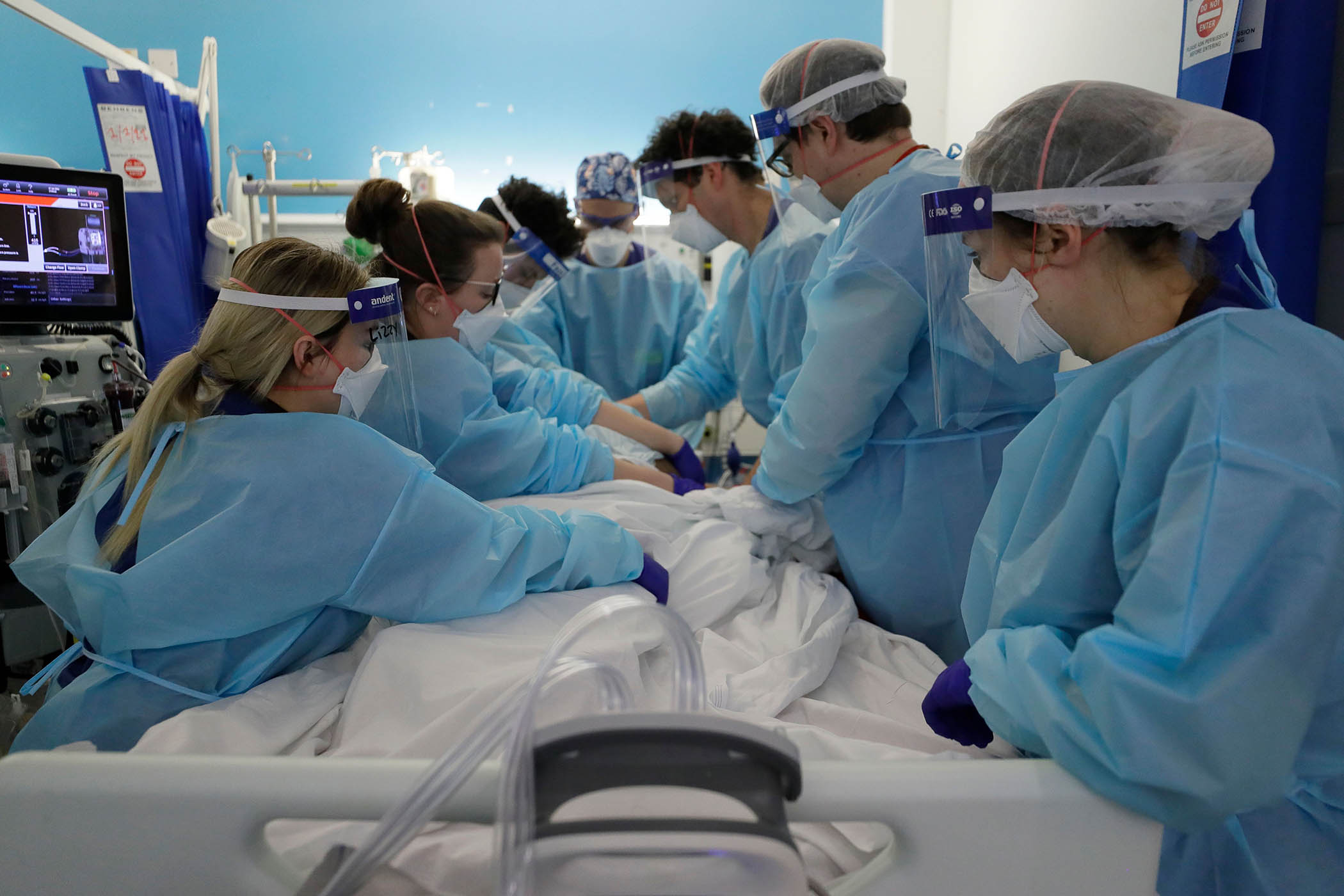
It is difficult to capture how deeply the pandemic affected our NHS teams. The numbers that we recorded in spreadsheets didn’t do it justice. What I saw in the hospitals we visited will always stay with me. These patients were among the sickest our teams had ever seen. They stayed in hospital longer, and they needed more equipment, interventions and staff time than those we would normally see outside the pandemic.
And they were, of course, more likely to die. Of the 37,000 Covid patients treated in intensive care in the first 18 months of the pandemic, half were under the age of 60 and a third would not survive to leave hospital. But even that doesn’t begin to describe what our frontline staff had to go through.
My teams visited more than 50 hospitals across England. I led more than 40 of the visits myself. The sheer scale of the death clinicians witnessed was shocking. One nurse told me that patients seemed to be “raining from the sky”; another that she simply got tired of putting people in body bags. Others told me of how they ran out of PPE and went to work wearing bin liners, or raided outdoor shops for waterproof trousers and cagoules. Nurses described vomiting on their way to work out of fear for what the day might bring.
At one ICU, nurses unable to leave their patients’ side took to wearing adult nappies because there weren’t enough staff for them to take toilet breaks. I’ll never forget the team who reported that their nurses had run out of body bags and were traumatised at having to put dead patients into clear plastic sacks and seal them with cable ties.
Newsletters
Choose the newsletters you want to receive
View more
For information about how The Observer protects your data, read our Privacy Policy
Much of this happened before vaccines were freely available, and the frontline teams didn’t escape infection. I visited more than one ICU where they had admitted staff from their own hospitals and teams, with a matron describing the day when 10 patients had died in 24 hours, two of her own colleagues among them.
Our visits focused on ICUs. But there were many places, right across the NHS, where conditions were as bad, if not worse. I wish we’d had the time and resources to do more. But like so much of Covid, it was the best we could do with what we had.
The NHS was never resourced or equipped to deal with a pandemic threat on the scale that Covid-19 brought. There was precious little capacity in the system on the day that the WHO declared Covid a global pandemic. And yet somehow we avoided total collapse.
That feat depended absolutely upon the NHS workforce and its ability to improvise, innovate and work around the insufficiencies they faced. It was the NHS personnel, more than any technical element of the response, that enabled the service to cope. It is this we must learn from – and never forget.
Covid unmasked the truth about the health service. The NHS is its people. They are its most valuable, adaptable and agile resource. But they too need looking after.
At one ICU, nurses unable to leave their patients took to wearing nappies, as there weren’t enough staff for them to take toilet breaks
At one ICU, nurses unable to leave their patients took to wearing nappies, as there weren’t enough staff for them to take toilet breaks
In 2022, a year after the worst wave of the pandemic had passed, more staff left the NHS than at any time in the history of the service, including one in nine of our nurses. Hallett makes it crystal clear in her report: “The impact of the pandemic on healthcare systems, their staff and their patients was devastating. We must never reach that point again.”
To minimise that risk, the inquiry makes many recommendations. It is imperative that our government delivers on them. Among these are the need for better mechanisms to reinforce infection control, and measures to improve the identification and care of people vulnerable to that infection. There is recognition, too, of where our response fell short: particularly in our overly restrictive visiting rules and how we handled care at the end of life. All of these lessons were hard won, and we must act upon them.
But it is the recommendations about configuring a system with the capacity to meet sudden increases in demand of the type created by the pandemic that need the most urgent response. These have the potential to protect us against future pandemic threats but also to improve the quality and quantity of care we provide every day.
That, however, will require brave political decisions, something highlighted by evidence from Prof Chris Whitty, chief medical officer for England, on the same day I gave mine. “You can have more capacity,” he said. “Taking ICU in particular, the UK has a very low ICU capacity compared with most of our peer nations. Now, that’s a choice. That’s a political choice. It’s [a] system configuration choice, but it is a choice.” And what we learned from Covid, to our great cost, was that our capacity to surge, to meet demand, lies in our workforce; that if you don’t have it now, you can’t magic it up in a crisis.
“Fundamentally,” said Whitty, “the limit to that system, as to any system, is trained people, and there is no way you can train someone in six weeks to have the experience of an experienced ICU nurse or an experienced ICU doctor. It is simply not possible. So if you don’t have it going into the emergency, if it’s an emergency of this speed of onset, you don’t have any illusions you’re going to have it as you hit the peak.”
The final recommendation of this module of the inquiry is of course close to my heart: a plea that we focus more carefully on the needs of the people upon whom the response to any healthcare crisis depends.
Hallett recommends that the system of peer support visits we developed during Covid – taking teams into hospitals to support those under the greatest strain, and helping close the gap between what senior leadership can glean from data and what is really happening on the shop floor – should be preserved. We will need that when we face the next pandemic. One could argue that we need it right now.
But we must go much further than that. The pandemic shows us that workforce wellbeing should become a central strategic priority for the National Health Service. For too long it has been a secondary consideration, when it needs to be front and centre. To do that we need better mechanisms to monitor, protect and promote the wellbeing of our frontline teams, both when they are in crisis and during everyday operation.
Covid taught us just how remarkable the people who work every day to deliver the care in our NHS really are. They should be deeply proud of what they did to shore up the NHS and protect it from collapse during the pandemic. But above all it showed us that we draw a false dichotomy between the needs of our patients and the needs of our staff. And that if we do not care for our carers, they will not be able to care for their patients.
Kevin Fong is a consultant anaesthetist, broadcaster and professor of public engagement and innovation in the Department of Science, Technology, Education and Public Policy at UCL
Photography by Kirsty Wigglesworth/AFP via Getty Images